This is part 2 of a 2-part VBAC birth story. You can read Part 1 on the birthED blog.
Now it was time to get down to business.
The nursing staff and a doctor who I didn’t have during my prenatals (my actual doctor happened to be on vacation when I went into labor) let me act on my natural urge to push. Unfortunately, I did not have an overwhelming sense to push but continued to contract and labor for almost two additional hours. My provider recommended that during a contraction, I start to push.
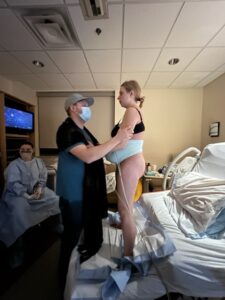 My doula, Ale, assisted my husband and I to get into different pushing positions and different places in the room to try pushing. We settled on a position that felt comfortable and natural to me.
My doula, Ale, assisted my husband and I to get into different pushing positions and different places in the room to try pushing. We settled on a position that felt comfortable and natural to me.
A nurse in my delivery room recommended a mirror to watch baby crown and help with mind-body connection.
At first, I declined, but then I decided to try it. The mirror ended up being an immense help and a great motivator during pushes.
My provider also recommended an artificial rupture of membranes (“AROM”) in order to increase the feeling of pressure of baby’s head right on my cervix.
I trusted my support staff and their recommendations, and agreed.
I actually remember that Savanna kept declining the artificial rupture of membranes (AROM). The reason the baby wasn’t giving her the deep pressure she was needing was probably more because of the baby’s position (occiput posterior, or “OP”). My memory is that Savanna’s water broke on its own after she declined the AROM a few times.
– Ale, Midwest Doulas
 My contractions started to space out and I was nodding off in between, feeling exhausted. At this point, I had been awake and in labor for over 24 hours. I was using every ounce of my being to push through contractions. I was running on fumes. I felt like I had nothing left to give.
My contractions started to space out and I was nodding off in between, feeling exhausted. At this point, I had been awake and in labor for over 24 hours. I was using every ounce of my being to push through contractions. I was running on fumes. I felt like I had nothing left to give.
With the encouragement of my husband, doula, hospital staff, and a small amount of Pitocin in my IV, things started to pick up again – and quickly.
The final push and “ring of fire” sensation totally took over my body. I could not fight it.
Finally, after 3 hours of pushing and 26 hours of labor, I got to hear the first cry of my sweet VBAC baby.
He was born “OP,” or occiput posterior position, where baby’s head is down, but facing mother’s front instead of her back.
I DID IT!
But more importantly, WE DID IT!
I was not surprised at all that this baby was OP, given the labor pattern of the day. Two of the nurses did come up to her afterwards and mentioned it was the coolest birth they had ever seen. It seemed like everyone learned something that day about the strength of this person and the ability to achieve a Vaginal Birth After Cesarean by surrounding the laboring person with trust and support.
– Ale, Midwest Doulas

It wasn’t just me in this process. It took my mind’s focus and my body’s energy. It took my baby’s cooperation. It required my husband’s unwavering support. It required my doula’s expertise and encouragement, my provider’s aid, and my nursing staff’s care to make this vaginal birth after cesarean (VBAC) birth possible.
What seemed like the perfect storm turned out to be the most challenging, yet empowering, emotional, and beautiful marathon of my life and it came with the greatest reward: my baby! I will forever wear this birth like a badge of honor.
If I could offer any advice for hopeful pregnant people looking for a VBAC: Trust the process. Trust that your body and baby were literally designed and created for birth. Trust yourself and your chosen support team. Trust that you can and WILL get a VBAC. You can do it!
If you are VBAC-hopeful, or even VBAC-curious and would like to have a free consultation to learn more about how Midwest Doulas can support you in your birth, please contact us.
If you’re interested in learning about how to prepare for VBAC, join birthED for one of their upcoming VBAC Prep workshops.









